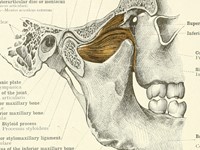
Massage Therapy for Temporomandibular Disorders
Massage Therapy for Temporomandibular Disorders
BlogImage
Temporomandibular Disorders (TMD) are not particularly uncommon, affecting up to 15% of adults and 7% of adolescents. Symptoms can include jaw pain, jaw stiffness or even locking and clicking of the jaw. Risk factors of developing TMDs include factors related to jaw function, such as functional overloading or specifics of a person’s bite, as well as psychosocial factors such as mental stress or work environment. TMDs can have a negative impact on mental health and can reduce quality of life.
Massage therapy can help people with TMDs relieve pain and improve jaw function.
Reducing Symptoms
Massage therapy can relieve the frequency and intensity of symptoms of TMDs. This includes a reduction in pain and tension that can be noticed immediately by some patients after an initial session, as well as improved range of motion in the jaw.
Manual therapies such as massage therapy, especially when combined with neck and jaw exercises can be even more effective in reducing jaw pain and can help improve jaw range of motion for people with temporomandibular disorders. Pain in the muscles used for chewing is common in people with temporomandibular joint disorders and a therapeutic exercise program that can be recommended by an RMT can help reduce the intensity of this sort of pain.
Don’t Forget the Head and Neck
TMDs are commonly associated with neck pain, which can affect more than half of people with TMDs. Massage therapy especially when combined with exercise recommendations can help provide relief from neck pain. Even on its own, massage therapy can be beneficial to people with chronic neck pain specifically.
People with TMDs also often experience chronic headaches. Massage therapy, especially when combined with therapeutic exercise, has been recommended to help people with chronic headaches reduce the frequency and intensity of their headaches.
Improving Function
TMDs can negatively impact jaw function, which can make a variety of things more difficult, including chewing, yawning, swallowing, and talking. Myofascial pain is a common symptom of TMD – it is often associated with the clenching of teeth, grinding and stress. In addition to pain, it can be associated with decreased ability to move the jaw comfortably, and massage therapy can re-establish the proper flexibility and muscular length as well as relieve pain.
TMDs are also associated with a lower quality of life especially due to the symptom of chronic pain and disruption in the ability to function. Massage therapy is a great option to provide some relief from chronic pain and can help people with TMDs improve their overall quality of life.
Temporomandibular Disorders can cause significant pain and have an impact on jaw function. Massage therapy can help people with TMDs find some pain relief and get back to their normal function.
References
Armijo-Olivo S, Pitance L, Singh V, Neto F, Thie N, Michelotti A. Effectiveness of Manual Therapy and Therapeutic Exercise for Temporomandibular Disorders: Systematic Review and Meta-Analysis. Phys Ther. 2016 Jan;96(1):9-25. doi: 10.2522/ptj.20140548. Epub 2015 Aug 20. PMID: 26294683; PMCID: PMC4706597.
Bitiniene D, Zamaliauskiene R, Kubilius R, Leketas M, Gailius T, Smirnovaite K. Quality of life in patients with temporomandibular disorders. A systematic review. Stomatologija. 2018;20(1):3-9. PMID: 29806652.
Defrin R. (2014). Chronic post-traumatic headache: clinical findings and possible mechanisms. The Journal of manual & manipulative therapy, 22(1), 36–44.
Eisensmith, L. P. (2007). Massage therapy decreases frequency and intensity of symptoms related to temporomandibular joint syndrome in one case study. Journal of Bodywork and Movement Therapies, 11(3), 223–230. https://doi.org/10.1016/j.jbmt.2007.03.001
Gil-Martínez A, Paris-Alemany A, López-de-Uralde-Villanueva I, La Touche R. Management of pain in patients with temporomandibular disorder (TMD): challenges and solutions. J Pain Res. 2018 Mar 16;11:571-587. doi: 10.2147/JPR.S127950. PMID: 29588615; PMCID: PMC5859913.
Kong LJ, Zhan HS, Cheng YW, Yuan WA, Chen B, Fang M. Massage therapy for neck and shoulder pain: a systematic review and meta-analysis. Evid Based Complement Alternat Med. 2013;2013:613279. doi: 10.1155/2013/613279. Epub 2013 Feb 28. PMID: 23533504; PMCID: PMC3600270.
Kuć J, Szarejko KD, Gołȩbiewska M. Smiling, Yawning, Jaw Functional Limitations and Oral Behaviors With Respect to General Health Status in Patients With Temporomandibular Disorder-Myofascial Pain With Referral. Front Neurol. 2021 May 24;12:646293. doi: 10.3389/fneur.2021.646293. PMID: 34108927; PMCID: PMC8182059.
Lee KS, Jha N, Kim YJ. Risk factor assessments of temporomandibular disorders via machine learning. Sci Rep. 2021 Oct 5;11(1):19802. doi: 10.1038/s41598-021-98837-5. PMID: 34611188; PMCID: PMC8492627.
List T, Jensen RH. Temporomandibular disorders: Old ideas and new concepts. Cephalalgia. 2017 Jun;37(7):692-704. doi: 10.1177/0333102416686302. Epub 2017 Jan 9. PMID: 28068790.
Moleirinho-Alves PMM, Cebola PMTC, Dos Santos PDG, Correia JP, Godinho C, Oliveira RANDS, Pezarat-Correia PLC. Effects of Therapeutic and Aerobic Exercise Programs on Pain, Neuromuscular Activation, and Bite Force in Patients with Temporomandibular Disorders. J Pers Med. 2021 Nov 10;11(11):1170. doi: 10.3390/jpm11111170. PMID: 34834522; PMCID: PMC8623244.
Odell, J., Clark, C., Hunnisett, A., Ahmed, O. H., & Branney, J. (2019). Manual therapy for chronic migraine: a pragmatic randomised controlled trial study protocol. Chiropractic & manual therapies, 27, 11.
Quinn, C., Chandler, C., & Moraska, A. (2002). Massage therapy and frequency of chronic tension headaches. American journal of public health, 92(10), 1657–1661.
Sherman KJ, Cherkin DC, Hawkes RJ, Miglioretti DL, Deyo RA. Randomized trial of therapeutic massage for chronic neck pain. Clin J Pain. 2009 Mar-Apr;25(3):233-8. doi: 10.1097/AJP.0b013e31818b7912. PMID: 19333174; PMCID: PMC2664516.
Silveira A, Gadotti IC, Armijo-Olivo S, Biasotto-Gonzalez DA, Magee D. Jaw dysfunction is associated with neck disability and muscle tenderness in subjects with and without chronic temporomandibular disorders. Biomed Res Int. 2015;2015:512792. doi: 10.1155/2015/512792. Epub 2015 Mar 26. PMID: 25883963; PMCID: PMC4391655.
Tchivileva IE, Ohrbach R, Fillingim RB, Greenspan JD, Maixner W, Slade GD. Temporal change in headache and its contribution to the risk of developing first-onset temporomandibular disorder in the Orofacial Pain: Prospective Evaluation and Risk Assessment (OPPERA) study. Pain. 2017 Jan;158(1):120-129. doi: 10.1097/j.pain.0000000000000737. PMID: 27984525; PMCID: PMC5639910.
Trize DM, Calabria MP, Franzolin SOB, Cunha CO, Marta SN. Is quality of life affected by temporomandibular disorders? Einstein (Sao Paulo). 2018 Nov 29;16(4):eAO4339. doi: 10.31744/einstein_journal/2018AO4339. PMID: 30517362; PMCID: PMC6276907.
Walczyńska-Dragon K, Baron S, Nitecka-Buchta A, Tkacz E. Correlation between TMD and cervical spine pain and mobility: is the whole body balance TMJ related? Biomed Res Int. 2014;2014:582414. doi: 10.1155/2014/582414. Epub 2014 Jun 19. PMID: 25050363; PMCID: PMC4090505.
Wieckiewicz M, Boening K, Wiland P, Shiau YY, Paradowska-Stolarz A. Reported concepts for the treatment modalities and pain management of temporomandibular disorders. J Headache Pain. 2015;16:106. doi: 10.1186/s10194-015-0586-5. Epub 2015 Dec 7. PMID: 26644030; PMCID: PMC4671990.